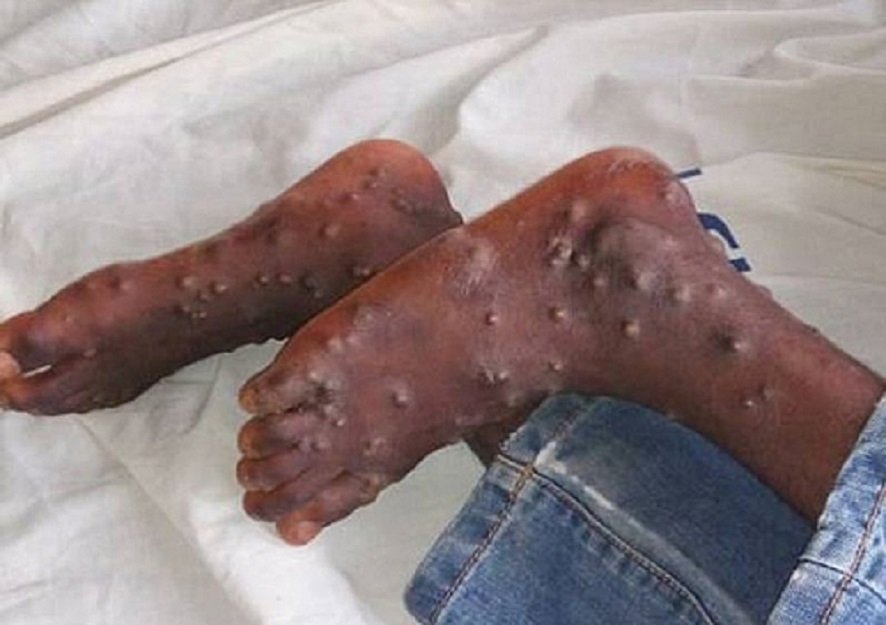
Monkeypox virus (MPXV) is a sporadic viral disease that is found predominantly in the rainforest countries of central and West Africa (CDC 2003), causing outbreaks in remote villages, where it is believed to result from close contact between humans and infected animals living in the rainforests.
According to Shchelkunov et al., 2001, MPXV causes a human disease that resembles smallpox but with a lower human to human transmission rate while vaccinia virus has been known to provide a cross-protection against Variola virus, which is the causative agent of smallpox, before its eradication in the late 70s.
For this reason, I engaged myself in the continuous research on poxvirus. It wasn’t a surprise when I heard about the recent outbreak of MPXV (Monkeypox virus) in Bayelsa State, Nigeria which has subsequently spread to places like Akwaibom, Lagos, Ekiti, Ogun, and Rivers state. This virus has been classified as the most virulent Zoonotic Orthopoxvirus which has affected human since the eradication of Variola virus (VARV).
Till date, the natural host of this virus, as well as its transmission cycle is not well known but there is still the notion that African rope squirrels (Funisciurus spp.) are considered a major reservoir. In my work on “Modified Vaccinia Virus Ankara (MVA) obtained by multiple serial passages on human cell line” (Offor C, 2015) where I deployed techniques like Plaque Assay, Cell culture Assay, Immunostaining, Cell Spreading Assay, Virus multiplication assay, PCR, Cell Permissivity Assay, RFLP analysis of virus genomes and High transmission electron microscopy.
I highlighted some various issues on MPXV (Monkeypox virus) as well as updating the total number of strains to 214 MPXV strains. MPXV first outbreak occurred in 1970 in Zaire (the present Democratic Republic of Congo (DRC) before spreading to other parts of the world including the United States. Hence this is not the first outbreak in Africa but the problem is how it’s been handled.
Currently, I do agree there are no known vaccines for the treatment of Monkeypox virus but based on my knowledge I do understand before exposure to MPXV, people need to be vaccinated with the known vectored vaccine which protected human subjects from smallpox infection in the late 70s.
It’s worrisome to know that the Nigeria health sector has not gotten to half the standard of western nations. So why can’t they vaccinate people with the vaccine produced from MVA since they are aware of the zoonotic nature of this virus and also the fact that vectored vaccines have some amount of protection against infections by Monkeypox if administered early on time?
Today in the northern part of Nigeria which has lots of camels which imply there is a possibility of the occurrence of Camelpox infection except if there is an absolute measure to prevent it. I have the feeling that the reason for non-reoccurrence of Camelpox today maybe as a result of smallpox vaccinations done many years ago which brings us to the fact that Camelpox virus and Variola virus (Causative agent of smallpox) are close relative as they share almost the same genetic makeup.
Hence, this is responsible for the inability of Camelpox to cause human disease. Consequently, genetic modification of Camelpox to delete genes that are present in Camelpox but absent in Variola virus doesn’t make sense
As an average Nigerian citizen will say “I reject it” If u like say u reject it but it’s just a reality”.
As far as am concerned Camelpox has become one of the most economically important Orthopoxvirus infections due to the dependence of many subsistence-level nomadic communities on camels. We need to wake up with advance scientific research!!!
Submitted By: Collins Obiorah Offor (MSc)